Regular check-ups for sexually transmitted infections (STIs) should be an essential part of your and your partner’s health. If you are looking to start a family, there is even more reason to make sure that there are no infections untreated.
Some people think that there is no need to check for STIs because there is “no chance” that they could’ve gotten one, but many STIs do not show symptoms and pose serious threat to fertility silently. It is estimated that 10-15% of women with chlamydia develop pelvic inflammatory disease (PID) due to untreated infections, which can damage their reproductive organs and make it harder to conceive. Some of these damages are irreversible and can render women infertile.
Therefore, it is important to be aware of the common types of STIs and know that asking for STI tests are nothing embarrassing or unnecessary, but crucial.
Chlamydia
Chlamydia is one of the most common types of STI that can remain undiagnosed for a long time due to lack of symptoms. When symptoms do occur, it is often too late as structural damages to the reproductive organs are done, which could be hard to repair.
Chlamydia first causes inflammation in the urethra and the cervix, which can then infiltrate through the uterus if left untreated. Eventually, the infection can extend to the fallopian tubes and ovaries, and cause PID.
Women with PID may experience chronic pain in the lower abdomen or pain during sexual intercourse. Since chronic PID can cause scarring and adhesions in fallopian tubes, it greatly increases the risk of tubal infertility and ectopic pregnancy because eggs or embryos could get stuck in the tubes. Ectopic pregnancies are life-threatening to the mother if bleeding occurs, which is estimated to cause 10% of pregnancy-related maternal deaths.
When detected early, chlamydia can be treated with a single dose of antibiotics. The treatment is so simple and effective, but can save you lots of frustration in the future.
Gonorrhoea
Gonorrhoea is similar to chlamydia in terms of lacking symptoms and causing PID in the long term. It can be transmitted through vaginal, oral and anal sex. In men, gonorrhoea can also damage the epididymis, which are tubes that transport sperm from testes to the ejaculate. Gonorrhoea is more prevalent in males, as opposed to affecting more females in the case of chlamydia.
Human immunodeficiency virus (HIV)
HIV is well known to affect immune functions and reduce patients’ overall health. It can be transmitted through sex, pregnancy and breastfeeding. Fortunately, anti-viral treatments are widely available for AIDS, and most parents are well educated on pregnancy planning to minimise the risk of mother-to-child transmission. The use of assisted reproductive technology offers favourable outcomes for HIV parents.
Herpes
Genital herpes is another common STI caused by the herpes simplex virus (HSV). Symptoms often include small, painful blisters, painful urine passing and vaginal discharge. In addition, three-quarters of women with herpes will experience at least one flare-up during pregnancy. During childbirth, HSV can also be transmitted to the baby through direct contact. As such, a caesarean section is often preferred in women with active lesions due to herpes.
Syphilis
Syphilis infection is not common but poses serious risk to a growing fetus during pregnancy. It leads to increased miscarriage risk and congenital abnormalities. Children born with congenital syphilis can have health problems later in life. Therefore, early detection and treatment with antibiotics are critical.
Summary
In summary, most STIs can lead to pelvic inflammation and damages the female fertility when left untreated. Unfortunately, many women find out their infections too late due to lack of symptoms, usually when they have trouble conceiving. The best solution is to have regular STI check-ups. Early detection and antibiotic treatment could very effectively prevent irreversible damage as well as circulation of STIs in the community.
Egg freezing – women’s chance to freeze time?
More than 95% of the Australian women are now aware that freezing eggs is an option for preserving their fertility. Although initially developed for cancer patients before they undergo chemotherapies, “social egg freezing” is becoming increasingly popular. When asked why, some women say that freezing their eggs was freezing their time.
Why egg freezing?
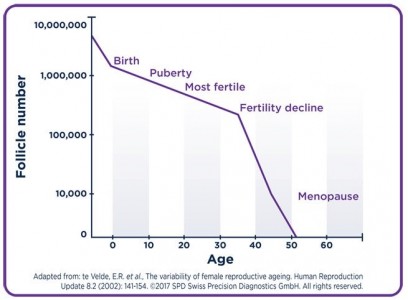
While men produce lots of sperm on a daily basis, women’s eggs adopt a quality over quantity strategy. Women are born with a set number of eggs that declines irreversibly. By their mid-30s, the egg reserve and quality really start to tank. This is when women go from fertile to subfertile, and eventually infertile when they hit menopause.
Unfortunately, this evolutionary design of the female reproductive timeframe isn’t compatible for many women. For example, they may not be ready for a baby, don’t want to pause their career trajectory, or simply haven’t met Mr.Right.
What’s involved in egg freezing?
The procedure involves hormonal stimulation that allows multiple eggs to mature. This requires you to inject prescribed hormonal medication every day for 10-12 days. You will be told do go into the clinic on a planned “egg pick up” date, where your doctor uses a transvaginal ultrasound-guided probe to aspirate (suck) eggs from the ovaries. Usually, you will be put under light general anaesthetic and can go home a few hours after the procedure.
Your part is done. The rest happens in the lab where scientists will put your eggs through a freezing procedure called vitrification. Vitrification by liquid nitrogen can keep the eggs good for years. You don’t need to worry about the eggs going bad. There is a baby born after being frozen as an embryo for 24 years.
What are the success rates?
Despite being a relatively new procedure, the figures that we have so far are quite encouraging. According to IVF Australia, you can expect these success rates:
- For women under the age of 35, one stimulated cycle allows collection of 10-12 eggs on average. 7-9 of these are suitable for freezing.
- 80-90% of the frozen eggs would survive thawing in the future
- About 50-80% of the thawed eggs would fertilise
- One embryo has a 20-35% chance of resulting pregnancy
As you can see, egg freezing itself has a promising success rate. It is the protracted journey of fertilisation to pregnancy that dramatically reduces the odds. However, rest assured that all this loss has been accounted for by collecting approximately 20-30 eggs.
Generally, success rates are higher for women younger than 35 as their quantity and quality of eggs are better. When women come in for egg freezing in their 40s, fertility preservation is unlikely to succeed because fertility is already very limited.
If you are considering egg freezing and not sure when, it’s a good idea to check your ovarian reserve with an Anti-Mullerian Hormone (AMH) test and reproductive organs with ultrasound. A fertility specialist such as Dr Alex Polyakov will be able to assess your fertility status using this information.
Can you rely on egg freezing?
Unfortunately, egg freezing does not guarantee a live birth. there are many factors that can get in the way of conceiving. As such, most women who freeze their eggs consider egg freezing and assisted reproductive technology as a backup plan. Their plan A is still to get pregnant naturally when the time is right. However, using assisted reproductive technology does offer the opportunity of preventative care in case you or your partner carries a genetic mutation that can be passed on.
Should you freeze your eggs due to COVID?
Many women are concerned that the coronavirus may affect their fertility. Until now, we have no scientific evidence to support this notion. Therefore, there is no need to rush into freezing your eggs for this reason, especially when you haven’t thoroughly researched about the implications and cost involved.